Gut microorganisms affect response to cancer treatment
24 November 2013
A healthy population of microorganisms that live off other microorganisms in the intestine is required for optimal response to cancer therapy, according to a study led by scientists at the US National Cancer Institute (NCI).
The researchers found that mice completely lacking these microorganisms (bred to be without), or mice treated with antibiotics to deplete the gut of bacteria, were largely impaired in their ability to respond to immunotherapy that slows cancer growth and prolongs survival.
The mice were also impaired in their ability to respond to mainstay chemotherapy drugs such as oxaliplatin and cisplatin. These findings in mice may underscore the importance of microorganisms in optimal cancer treatment outcomes in humans.
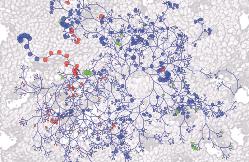
Image of an evolutionary tree of mouse gut
bacteria
superimposed over an image of colon tissue with
larger circles indicating greater abundance of bacteria.
Red
circles are bacteria that prime mice to respond
to
immunotherapy; green shows bacteria that suppress
anti-tumor
response to the drug.
Gut commensal microbiota are microorganisms that live in the gut and thrive but do not affect their host — in this study laboratory mice. Humans also harbour gut commensal microbiota that can influence local and body-wide inflammation as well as modify the tumour microenvironment, which consists of cells, signalling molecules and mechanisms that may support tumour growth and also cause drug resistance.
To study the importance of commensal bacteria, the scientists used mice raised in sterile conditions from birth so they did not harbour any bacteria, or alternatively, conventionally raised mice that received a potent antibiotic cocktail that is known to decrease bacteria by more than 10,000–fold. The mice received these antibiotics in their drinking water, starting three weeks prior to tumour inoculation. They continued to receive doses of the antibiotic cocktail throughout the experiment.
To analyze tumours at comparable stages of progression, lymphoma, colon, and melanoma cancers that could be transplanted were selected, based on their susceptibility to therapeutic drugs. Cancer cells from these tumours were then injected under the skin of the mice, where they formed tumours that grew to reach a diameter of one-fifth of an inch or more. The tumours were then treated with an immunotherapy that included CpG-oligonucleotides, which stimulated the immune system, or with the chemotherapy drugs oxaliplatin and cisplatin, which attacked the tumours.
Germ-free mice, or mice that received the antibiotic cocktail, responded poorly to drug therapy for their tumours. This resulted in a lower production of cytokines (proteins secreted by lymph cells that affects cellular activity and controls inflammation) as well as lower tumour death therefore demonstrating that optimal responses to cancer therapy required an intact commensal microbiota.
In an independent co-submitted study that will appear in the same issue of Science, Laurence Zitvogel MD PhD, Gustave Roussy Institute, Paris, and colleagues showed that a different type of chemotherapy drug, cyclophosphamide, altered the composition of the intestinal microbiota and damaged the intestinal wall, thereby affecting optimal anti-tumour immune response and the therapeutic effectiveness of cyclophosphamide.
“The use of antibiotics should be considered as an important element affecting microbiota composition. It has been demonstrated, and our present study has confirmed, that after antibiotic treatment the bacterial composition in the gut never returns to its initial composition,” said Trinchieri. “Thus, our findings raise the possibility that the frequent use of antibiotics during a patient’s lifetime or to treat infections related to cancer and its side-effects may affect the success of anti-cancer therapy.”
In next steps, Goldszmid and Trinchieri will work in mice to fully characterize the molecular signalling by which the bacteria in the gut can actually send messages to distant organs or tumours and change the type and level of inflammation present in those organs. They also plan to characterize, in humans, the role of gut bacteria on the bodies’ inflammatory response and tumour response to therapy. Additionally, the researchers plan to design clinical studies by giving antibiotics to healthy volunteers to study their effect on the molecular mechanisms regulating inflammation.