Microscope detects cancer cells spreading through the bloodstream
1 October 2013
A team at Stanford University is developing a pen microscope that could noninvasively detect cancer seed cells circulating in the bloodstream, allowing for earlier interventions than current techniques.
Currently, a blood sample is analysed using special antibodies to detect the presence of these seed cells, called circulating tumour cells (CTCs). This works well if CTCs are present in large numbers, but may fail to detect smaller numbers in the early phase of tumour growth.
In the new technique, a patient is injected with a dye that causes the CTCs to fluoresce. A pen-sized microscope focusses a low-power laser light on a blood vessel just a few hair-widths below the patient's skin.
As the dyed cancer cells pass through the laser, the light excites them and causes them to stand out from normal cells. The microscope registers each of these cells and a computer logs each observation. The improved sensitivity of the technology and the ability to noninvasively scan blood for long periods will help create a fuller picture of the number of CTCs in a person's body.
To date, the research has focused on developing the method in mice, taking advantage of the thin transparent tissue of the ear to image fluorescent cells traversing the small blood vessels below the skin.
"There has been a huge push to increase sensitivity," said Bonnie King, an instructor at Stanford School of Medicine. "We suspect that CTCs often circulate in numbers below our current threshold of detectability."
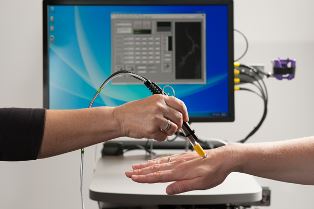
A pen-sized microscope focuses a low-power
laser light on a
blood vessel just below the patient's skin to
register dyed
cancer cells. (Photo credit: Linda A. Cicero / Stanford
News Service)
A major advantage with the microscopic technique, King said, is the ability to screen much larger volumes of blood, rather than just a small vial collected from a patient. This will be done using a method called in vivo flow cytometry, a laser-based technology for counting cells in a live subject.
"At present we will not screen all of a person's blood [with the microscope], but we are aiming to increase the amount of blood screened compared to a 7-milliliter blood draw," said Christopher Contag, Professor of Pediatrics at the School of Medicine.
The work is a collaborative effort of Olav Solgaard, a professor of electrical engineering; Geoffrey Gurtner, a professor of surgery; and Michael Clarke, a professor of oncology.
Soon the researchers will move the microscope to a clinical setting to conduct a proof-of-principle test of the technique in humans. Gurtner is currently conducting a clinical trial to evaluate the FDA-approved green dye for defining skin vasculature during post-mastectomy breast reconstruction surgeries. The researchers are piggybacking on this trial to test the miniature microscope's ability to detect blood vessels and circulating cells.