Skin cells converted directly into beating heart cells
16 Feb 2011
The Scripps Research Institute has developed a technique to convert adult skin cells directly into beating heart cells efficiently without having to first go through the laborious, time consuming and highly inefficient process of generating embryonic-like stem cells.
The powerful general technology platform could lead to new treatments for a range of diseases and injuries involving cell loss or damage, such as heart disease, Parkinson’s, and Alzheimer’s disease.
The work has been published in Nature Cell Biology [1].
"This work represents a new paradigm in stem cell reprogramming," said Scripps Research Associate Professor Sheng Ding PhD who led the study. "We hope it helps overcome major safety and other technical hurdles currently associated with some types of stem cell therapies."
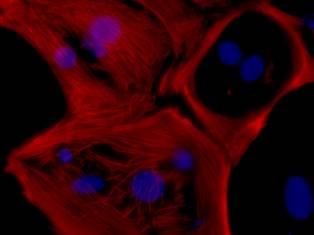
Mature heart muscle cells created directly from
skin cells
Making stem cells
As the human body develops, embryonic-like stem cells multiply and transform themselves into more mature cell types through a process known as differentiation, producing all of the body’s different cell types and tissues. Past the embryonic stage, however, the human body has limited capacity to generate new cells to replace ones that have been lost or damaged.
Thus, scientists have been trying to develop ways to “reprogram” adult human cells back to a more embryonic-like, or pluripotent, state, from which they are able to divide and then change into any of the body’s cell types. Using these techniques, scientists aim to someday be able to take a patient’s own cells, say skin cells, change them into heart or brain cells, and then insert them back into the patient to fix damaged tissues. In 2006, Japanese scientists reported that they could reprogram mouse skin cells to become pluripotent simply by inserting a set of four genes into the cells.
Although the technology to generate these cells, dubbed induced pluripotent stem (iPS) cells, represents a major advance, there are some hurdles to overcome before it can be adapted to therapies.
“It takes a long time to generate iPS cells and then differentiate them into tissue-specific functional cell types," said Ding, "and it’s a tedious process. Also, what you generate is not ideal.”
Specifically, it takes some two to four weeks for scientists to create iPS cells from skin cells and the process is far from efficient, with only one cell out of thousands making the complete transformation. Furthermore, once scientists obtain iPS cells, they then have to go through the tricky procedure of inducing the iPS cells to differentiate into desired types of cells, which takes an additional two to four weeks.
In addition, the process of generating mature cells from iPS cells is not foolproof. When, for example, scientists induce iPS cells to become heart cells, the resulting cells are a mix of heart cells and some lingering iPS cells. Scientists are concerned that giving these new heart cells (along with the remaining pluripotent cells) to patients might be dangerous. When pluripotent cells are injected in mice, they cause cancer-like growths.
Because of these concerns, Ding and colleagues decided to try to tweak the process by completely bypassing the iPS stage and going directly from one type of mature cell (a skin cell) to another (a heart cell).
Bypassing the stem cell stage
The team introduced the same four genes initially used to make iPS cells into adult skin fibroblast cells, but instead of letting the genes be continuously active in cells for several weeks, they switched off their activities just after a few days, long before the cells had turned into iPS cells. Once the four genes were switched off, the scientists gave a signal to the cells to make them turn into heart cells.
“In 11 days, we went from skin cells to beating heart cells in a dish,” said Ding. “It was phenomenal to see.”
Ding points out the protocol is fundamentally different from what has been done by other scientists in the past and notes that giving the cells a different kind of signal could turn them into brain cells or pancreatic cells.
“It is like launching a rocket," he said. "Until now, people thought you needed to first land the rocket on the moon and then from there you could go to other planets. But here we show that just after the launch you can redirect the rocket to another planet without having to first go to the moon. This is a totally new paradigm.”
In addition to better understanding the basic biology of stem cells, the next step will be to modify this technique further to remove the need for inserting the four genes, which have been linked to the development of cancer.
As a result, many scientists, including Ding, have been working on new techniques to develop iPS cells without use of these genes. That has proven difficult. But with the new protocol, which bypasses the iPS cell stage, the genes are needed for a much shorter time.
“Action for such a short period of time is a lot easier to replace,” Ding noted.
Reference
1. Jem A. Efe, Simon Hilcove, Janghwan Kim, Hongyan Zhou,
Kunfu Ouyang, Gang Wang, Ju Chen, and Sheng Ding. Conversion of
mouse fibroblasts into cardiomyocytes using a direct reprogramming
strategy"
Date: Published online January 30, 2011.