Radiologists diagnose appendicitis remotely by using smart phone
1 December 2009
Radiologists can accurately diagnose acute appendicitis from a remote location with the use of a handheld device or mobile phone equipped with special software, according to a study presented at the annual meeting of the Radiological Society of North America (RSNA) this week.
"The goal is to improve the speed and accuracy of medical diagnoses, as well as to improve communications among different consulting physicians," said the study's lead author, Asim F. Choudhri, M.D., fellow physician in the Division of Neuroradiology at Johns Hopkins University in Baltimore. "When we can make these determinations earlier, the appropriate surgical teams and equipment can be assembled before the surgeon even has the chance to examine the patient."
Appendicitis, or inflammation and infection of the appendix, is a medical emergency requiring surgical removal of the organ. Undiagnosed or left untreated, the inflamed appendix will rupture, causing toxins to spill into the abdominal cavity and potentially causing a life-threatening infection. Appendicitis can occur at any age but is most common in people between the ages of 10 and 30, according to the US National Institutes of Health.
Typically, a patient arriving at the emergency room with suspected appendicitis will undergo computed tomography (CT) and a physical examination. If a radiologist is not immediately available to interpret the CT images or if consultation with a specialist is needed, diagnosis is delayed, increasing the risk of rupture. Transmitting the images over a mobile device allows for instant consultation and diagnosis from a remote location. It can also aid in surgical planning.
"This new technology can expedite diagnosis and, therefore, treatment," Dr. Choudhri said.
 For
the study performed at the University of Virginia in Charlottesville, CT
examinations of the abdomen and pelvis of 25 patients with pain in the
right lower abdomen were reviewed over an encrypted wireless network by
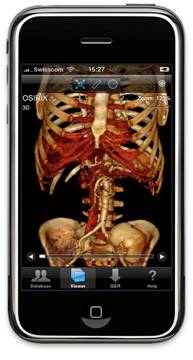
five radiologists using an iPhone G3 equipped with OsiriX Mobile medical
image viewing software. (Image on right shows an example of the Osirix
DICOM Viewer on Apple iPhone).
For
the study performed at the University of Virginia in Charlottesville, CT
examinations of the abdomen and pelvis of 25 patients with pain in the
right lower abdomen were reviewed over an encrypted wireless network by
five radiologists using an iPhone G3 equipped with OsiriX Mobile medical
image viewing software. (Image on right shows an example of the Osirix
DICOM Viewer on Apple iPhone).
All of the patients had surgical confirmation or follow-up evaluations to confirm whether or not they had appendicitis.
"The scans can be read in full resolution with very little panning, and the software allows the reader to zoom and adjust the contrast and brightness of the image," Dr. Choudhri said. "The radiologist is evaluating actual raw image data, not snapshots."
Fifteen of the 25 patients were correctly identified as having acute appendicitis on 74 (99 percent) of 75 interpretations, with one false negative. There were no false positive readings. In eight of the 15 patients who had appendicitis, calcified deposits within the appendix were correctly identified in 88 percent of the interpretations.
All 15 patients had signs of inflammation near the appendix that were correctly identified in 96 percent of interpretations, and 10 of the 15 had fluid near the appendix, which was correctly identified in 94 percent of the interpretations. Three abscesses were correctly identified by all five readers.
"The iPhone interpretations of the CT scans were as accurate as the interpretations viewed on dedicated picture archiving and communication system (PACS) workstations," Dr. Choudhri said.
Dr. Choudhri pointed out that patient privacy concerns would have to be addressed before any handheld mobile device could be considered practical for clinical use, but noted that this technique has great potential for improving emergency room care.
"We hope that this will result in improved patient outcomes, as evidenced by decreased rates of ruptured appendicitis, shorter hospital stays and fewer complications," he said.