| General care | |||||||
Ultrasound opens cell membranes for drug delivery12 September 2006 Ultrasound can open holes in cell walls large enough to allow large drug molecules to pass through, and the cells can repair the holes within minutes, according to research carried out by the Georgia Institute of Technology and Emory University. Understanding this mechanism could advance the use of ultrasound for delivering gene therapies, targeting chemotherapy and administering large-molecule drugs that cannot readily move through cell membranes.
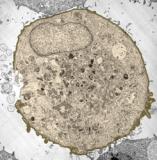
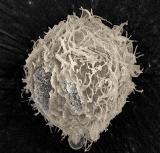
Using five different microscopy techniques, the researchers showed that the violent collapse of bubbles created by the ultrasound opens holes in the membranes of cells suspended in a liquid medium. The holes, which are closed by the cells in a matter of minutes, allow entry of therapeutic molecules as large as 50 nanometers in diameter — larger than most proteins and similar in size to the DNA used for gene therapy. “The holes are made by mechanical interaction with the collapsing bubbles,” said Mark Prausnitz, a professor in the School of Chemical and Biomolecular Engineering at the Georgia Institute of Technology. “The bubbles oscillate in the ultrasound field and collapse, causing a shock wave to be released. Fluid movement associated with the resulting shock wave opens holes in the cell membranes, which allow molecules from the outside to enter. The cells then respond to the creation of the holes by mobilizing intracellular vesicles to patch the holes within minutes.”
The research was reported in the journal Ultrasound in Medicine and Biology (Vol. 32, No. 6) and was supported by the National Institutes of Health (NIH) and the National Science Foundation (NSF). Ultrasound is the same type of energy already widely used for diagnostic imaging. Drug delivery employs higher power levels and different frequencies, and bubbles may be introduced to enhance the effect. Ultrasound drug delivery could be particularly attractive for gene therapy, which has successfully used viruses to insert genetic material into cells — but with side effects. It could also be used for more targeted delivery of chemotherapy agents. “One of the great benefits of ultrasound is that it is noninvasive,” Prausnitz said. “You could give a chemotherapeutic drug locally or throughout the body, then focus the ultrasound only on areas where tumours exist. That would increase the cell permeability and drug uptake only in the targeted cells and avoid affecting healthy cells elsewhere.” Researchers have only recently found that the application of ultrasound can help move drugs into cells by increasing the permeability of cell membranes. It had been hypothesized, but not definitively shown, that the ultrasound increased the permeability by opening holes in cell membranes.
Prausnitz and collaborators Robyn Schlicher, Harish Radhakrisha, Timothy Tolentino, Vladimir Zarnitsyn of Georgia Tech and Robert Apkarian (now deceased) of Emory University set out to study the phenomenon in detail using a line of prostate cancer cells. They used scanning and transmission electron microscopy of fixed cells and two types of optical microscopy of living cells to assess ultrasound effects and cell responses. Beyond demonstrating that ultrasound punched holes in cell membranes, the researchers also studied the mechanism by which cells repair the holes. After the ultrasound exposure, they introduced into the cell medium a chemical not normally taken up by the cells. By varying when the chemical was introduced, they were able to determine that most of the cells had repaired their membranes within minutes. Though the researchers used prostate cancer cells in the study reported in the journal, they have also studied other types of cells and believe ultrasound offers a general way to briefly create openings in many classes of cells. Researchers face a number of challenges, including FDA approval, before ultrasound can be used to deliver drugs in humans. For example, the effects of the ultrasound were not consistent across the entire volume of cells, with only about a third affected. Researchers will also have to address safety concerns and optimize the creation of collapsing bubbles – a phenomenon known as cavitation – within bodily tissues. “Before we can use ultrasound for therapy in the body, we will have to learn how to control the exposure,” Prausnitz noted. “If we can properly design the impact that ultrasound makes on a cell, we can generate an impact that the cell can deal with. We want just enough impact to allow transport into the cell, but not so much of an impact that the cell would be stressed beyond its ability to repair the injury.” Researchers don’t yet know if the membrane holes cause long-term harm to the affected cells. General assays show that cells survive after resealing the membrane holes, but detailed studies of cell behavior are still needed. Evidence from other researchers suggests that cell membranes are frequently damaged and repaired inside the body – without long-term ill effects. That suggests cells may similarly tolerate ultrasound’s effects. “One of the real challenges is going to be translating the successes that have occurred in the laboratory and in small animals into clinical success in people,” said Prausnitz. “Now that we better understand the mechanism of ultrasound’s effects, we can more effectively take advantage of it for medical therapy.”
|