Telemedical ECGs put into practice
Can you improve patient cardiac care and working practice for GP clinicians whilst reducing the cost of cardiac care to the NHS? GP, Dr Jonathan Lieberman, describes how a telemedical ECG service has done just this at his GP practice in Manchester, UK and outlines the benefits it has brought to patient, doctor and the NHS.
22 September 2011
When a patient comes into your surgery complaining of chest pains what do you do? Do you carry out an in-surgery test using a conventional ECG machine and interpret the results yourself? Or do you immediately refer them to hospital for an ECG test?
This is a common scenario faced by doctors in general practice. It is likely that many doctors don’t have access to in-surgery ECG machines, and those who do probably don’t have skilled ECG interpreters available to analyse the results which often means a majority of patients are sent to hospital for diagnostic tests.
Heart disease is one of the United Kingdom’s biggest killers. It is therefore unsurprising to learn that the cost of diagnosing, treating and caring for patients with cardiac related problems such as coronary heart disease (CHD) represents the single heaviest financial burden on the NHS every year, with an estimated £34 billion spent on cardiac care annually.
Delivering effective yet efficient cardiac care is something the Department of Health is focusing on and their National Service Framework for Coronary Heart Disease initiative includes standards for improving prevention, diagnosis and treatment of CHD. Finding a single solution that helps reduce the operational and financial burden of cardiac care on the NHS and delivers distinct benefits to both patients and their doctors would be the ideal answer.
Diagnosing the problem
Early detection should lead to early action, and moving diagnosis away from acute hospitals into primary care settings would be the optimum solution. Developing a more proactive and preventative model of care in a primary care setting would ease some of the financial and operational pressures placed upon acute care providers, not only benefiting patients from a clinical point of view but also frees up resources in secondary care.
The most common method of diagnosing cardiac conditions is the electrocardiograph [ECG] and whilst most GP surgeries have access to ECG machines, the skills required for accurate and detailed 12 lead ECG analyses can be difficult to maintain outside cardiology or emergency medicine specialities.
Telemedical ECGs import the same kind of cardiac expertise found in hospitals into a GP’s surgery, and coupled with a cardiac monitoring service that expertly interprets the results, it provides patients with a facility that not only gives them a full on-the-spot ECG test and assessment, but also cuts out the often lengthy waiting times that go hand-in-hand with hospital ECG tests.
Telemedicine in primary care — ECGs explained
St Gabriels Medical Centre in Prestwich, Greater Manchester, provides care for over 8,500 patients. Since 2006 the surgery has been using telemedical ECG services from Manchester-based telemedicine specialist Broomwell HealthWatch.
The NHS accredited cardiology reporting service provides quick expert diagnosis of chest-pain symptoms from trained cardiologists and has proven to be very popular with both patients and staff at the surgery. Incredibly easy to use, the service transmits 12 lead ECGs in just seconds to the monitoring centre where a cardiology clinician provides an immediate interpretation and returns the analysis report back to the GP.
Reaping the benefits
The reporting service and telemedical ECGs have greatly benefited St Gabriels Medical Centre. Although we have access to a conventional 12-lead ECG machine, staff were not 100% confident in interpreting the result and introducing the service has eased the pressure on them.
An additional benefit of the device is its portability. The new machines are much smaller hand-held devices compared to the traditional bulky ECG machines, allowing clinicians to use them in several different rooms within the practice with the potential to be used for home visits.
Response from patients has been overwhelmingly positive. Being able to stay within the familiar surroundings of their doctor’s surgery with faces they recognise and trust means they are more at ease. Having an ECG done at their local surgery also means they do not spend time travelling back and forth to hospital, meaning less hassle and reduced stress.
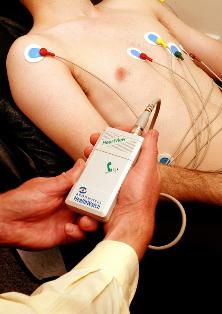
Taking an ECG
Proof is in the pilot
The burden of ‘frequent flyer’ patients on hospitals is considerable. Cutting unnecessary emergency admissions and referrals to outpatient clinics would free up hospital resources and accrue savings, which could be reallocated to other key areas.
A major two-year pilot carried out by the Greater Manchester and Cheshire Cardiac and Stroke Network (GMCCSN) revealed that Broomwell’s ECG service could prevent approximately 63% of referrals to secondary care if rolled out across the Network. The pilot, which started in 2007, enabled over 2,000 people to avoid a trip to hospital, saving the NHS thousands in care costs and eliminating patient delays, stress and anxiety through quicker, more convenient diagnosis.
Since deploying the telemedical ECG service at the medical centre, approximately 90% of patients who have come in for a test avoided going onto hospital and were offered reassurance at the surgery. Without the service these patients would have been sent directly to hospital, unnecessarily consuming NHS time and resources.
The successful outcomes of the initiative mean that healthcare bodies are beginning to realise the potential benefits of telemedicine and today the monitoring service is in use across 10 PCTs in Greater Manchester, as well as a large number elsewhere.
Watching arrhythmias
Telemedicine services are also beneficial as a diagnostic aid for other medical conditions, as a solution to further reduce cardiac referrals onto secondary care, saving patients a great deal of inconvenience and worry and reducing financial burden on the NHS.
Broomwell HealthWatch has recently launched the new Arrhythmia Watch, which captures and records episodes of arrhythmia as they are occurring. Worn on the wrist, the Arrhythmia Watch looks like a conventional sports watch, but can record a 1-lead ECG in just 40 seconds at the press of a button when the wearer feels symptoms of an arrhythmia.
Once the patient has captured suspected episodes of arrhythmia, the patient then returns to their GP surgery. The ECG results are downloaded from the watch and transmitted to Broomwell’s Cardiac Monitoring Centre, where a team of expert cardiac clinicians interpret the ECG trace, provide a precise diagnosis and return it to the GP.
The prognosis for telemedicine
The deployment across Greater Manchester and numerous other PCTs, positive feedback from telemedicine initiatives and research data all point to the overriding benefits of the telemedicine service to the patient, doctor and to the NHS. Experiences in using a telemedical service are a further testament to that.
Practice clinicians at the centre have generally been very positive about telemedical ECGs and agree they are a good diagnostic aid, which benefits patients and secondary care. However at a primary level, time and costs can be cause for concern. Performing ECG tests in-surgery can take up additional staff time and to fully realise the benefits, PCTs should consider allocating additional sums to cover the extra nursing time required.
Cardiac telemedicine is an excellent way to ensure that expert advice is available in a matter of minutes. Having access to instant diagnostic expertise helps us better perform our role as a doctor and instant results means the appropriate action can be taken quickly, helping us to deliver an optimal level of care to our patients.
Prevention, they say, is better than cure. Telemedical services undoubtedly prevent unnecessary hospital visits for patients who do not have a life-threatening condition. It also prevents a patient’s serious condition from worsening by ensuring they receive timely care. This proactive and preventative model of care has brought the expertise of cardiologists straight into the heart of primary care, helping to ensure NHS resources are optimised and used as effectively as possible whilst giving us the tools to provide the highest standard of care for our patients.
Dr Jonathan Lieberman
General Practitioner, St Gabriels
Medical Centre, Manchester